
Foal Septicaemia
A page about foal septicaemia describing cause, clinical signs, diagnosis and control.

Introduction
Foal septicaemia is defined as the presence of whole bacteria or bacterial components within the bloodstream of the neonatal animal. The contamination of the foal can occur before or just after birth and Gram negative aerobic bacteria are the most frequently isolated organism.
Aetiology
Due to the differences between the human and equine placenta and the environment in which mares give birth, the incidence of sepsis in the equine neonate is relatively high and foal septicemia (FS) is considered to be the main cause of death for foals within the first week of life. The single most important factor for the development of FS is the absorption of contaminated material through the foal gut in the early stages of extra-uterine life. Up to 18-24 hours after birth, the foal’s gut is able to absorb large molecules (>70.000 molecular weight) unchanged. This allows the foal to absorb antibodies passed from the dam through the colostrum, but also any other large molecules present, including bacteria.
Since the absorption of large molecules speeds up the closure of the gut, the delayed ingestion of colostrum coupled with increased ingestion of contaminated material during udder searching are the main causes of FS.
The most frequently encountered pathogens in FS are enterobacteriacee (Salmonella, Shigella, Escherichia, Klebsiella, Enterobacter etc.) but mixed infections are still frequent. Other pathogens may be involved in 30% of the cases (mixed infections) such as: Actinobacillus spp., Staphylococcus and Streptococcus spp. and anaerobes such as Clostridia and Bacteroides spp.
Epidemiology
Foal septicemia is the leading cause of death in foals in the first week of age. It accounts for 33% of foal mortality and, in the first week of life, is the second most frequently diagnosed disease after failure of immunity transfer.
Factors influencing incidence include:
a)OVERWHELMING INFECTION PRESSURE IN YOUNG LIFE
This relates to stable hygiene, navel management and management of the mare – factors that influence the levels of bacteria to which foals are exposed to in young life
b)FAILURE OF PASSIVE TRANSFER OF IMMUNITY
(i) Colostrum ingested too late – after 12 hours the ability of the foal to absorb antibodies declines
(ii) Colostrum production (quality and/or quantity) inadequate – Influenced by mare health, nutrition, genetics etc.
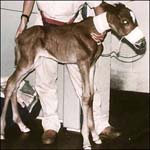
Clinical Signs
The clinical signs of (Foal septicaemia) FS are variable and often subtle, but it is paramount that therapy starts as soon as possible. The foals can appear apathetic, lethargic and not able to stand unassisted, but frequently they appear absolutely normal with no clinical signs whatsoever except for injected mucous membranes and a delayed capillary refill time. The Capillary refill time is an empirical method used to assess peripheral circulation. It is measured by applying pressure with your finger on the gingival mucosa and calculate the time required for the mucosa to return to the original pink colour (normal <2 secs). Injected mucous membranes (generally sclerae) occur where blood vessels are clearly visible. As the disease progresses, the foal may show evidence of single or multiple organ dysfunction. Sepsis can manifest itself as respiratory distress, pneumonia, diarrhoea, uveitis, meningitis, osteomyelitis or septic arthritis.
Within the affected foals, mortality ranges between 28 and 75% although there appears to be no relationship in race starts or earnings achieved whether yearlings were affected or not by FS when they were foals. This means that it is worthwhile to invest money in treating the affected foals, since foals that overcome FS are not necessarily weakened by the disease and can have a full life thereafter.
Diagnosis
Typically, the first assessment of the foal is done by the farm manager (just after parturition) or by the vet the following morning. At that time, the level of IgG are assessed and corrected if necessary by administration of either colostrum orally (< 18 hr from birth) or plasma i.v. The importance of an experienced person (manager or vet) in the early recognition of neonatal diseases cannot be overstated.
The decision may be taken to refer the foal to a Neonatal Intensive Care Unit (NICU) based on the sepsis scoring systems developed in 1988 (Koterba scoring system). The sepsis scoring system assigns numerical values to a number of clinic-pathological variables (fibrinogen, neutrophil count, IgG test, fever, attitude, etc.), including data from the dam (gross appearance of the placenta, duration of delivery, length of pregnancy). The first sepsis score system developed was able to correctly predict the presence of sepsis in 93% of cases and correctly predict the absence of it in 88% of cases. Subsequently, scoring systems have been found to be beneficial in also predicting the survival rate of referred foals.

Control
Supportive therapy is the first step in the treatment of foal septicaemia (FS). Thus, fluid therapy, naso-gastric or parenteral feeding, oxygen therapy and thermal regulation are of paramount importance to stabilize the foal prior to any other therapy. As stated above, supplementation with antibodies can be done both orally and parenterally, depending on the age of the foal. This is carried out until the foal has an antibody concentration of at least 800 mg/dl of plasma.
Since antibiotic therapy usually has to start before the causative organism can be identified, foals suspected of being septic should be placed on broad-spectrum antibiotics active against both Gram-positive and Gram-negative organisms. A fourth- generation cephalosporin is the only antibiotic specifically licensed for foal septicaemia treatment though other antibiotics may also be effective. Consult your vet for details.
Non-steroidal anti-inflammatory drugs (NSAIDs) are often used to decrease temperature and fight endotoxemia. In septicemic foals, it is customary to treat preventively for gastric ulcers using sucralfate in combination with a proton pump inhibitor (omeprazole).
Unfortunately there is currently no vaccine licensed for FS.
Recovery from neonatal sepsis depends not only on the severity and manifestation of the infection, but also on the speed with which the condition has been identified and the appropriate therapy has been initiated.
Currently, survival rates are up to 80% in referral centers, but a minimum of 1-4 wk of intensive care should be expected.
