
Ear Disease
A page about canine ear disease describing cause, clinical signs, diagnosis and control.
Introduction
Otitis externa, commonly referred to as “Canker”, is one of the most common dog ear problems and simply involves inflammation of the ear canal. Otitis externa affects approximately 1 in 5 of all dogs in Ireland and is most common in young dogs (aged 2-4 years).

Aetiology
Otitis externa (OE) is classically underpinned by factors that directly cause disease and those that either predispose to disease or perpetuate it. The latter two clusters of factors are further evaluated under the epidemiology section. A number of causal agents lead to OE directly with no need for any assistance from other factors as follows:
a) Parasites including fleas, ticks and mites can all lead to development of ear disease
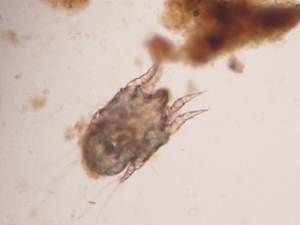
b) Fungal infections e.g. ringworm
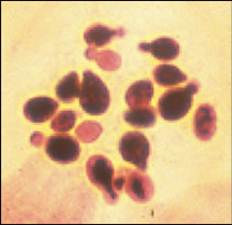
c) Allergies – Caused by a reaction to inhaled allergens (Atopy), food, contact with materials or drugs that the animal reacts to, the clinical presentation of disease may be OE which may or may not be accompanied by scratchy skin disease in other areas e.g. the paws.
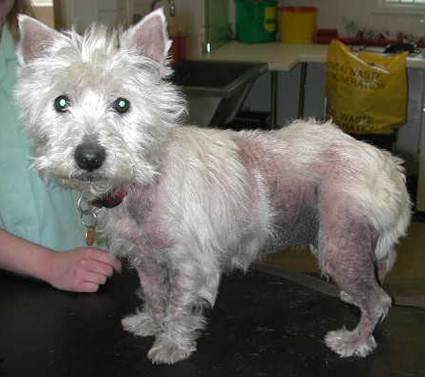
d) Foreign bodies – Something falling into the ear and becoming lodged there e.g. grass seeds, can lead to significant discomfort and OE
Epidemiology
A number of factors can increase the risk of developing Otitis Externa while others worsen disease or prolong it.
Predisposing factors include:
a) Anatomy – Pendulous pinnae, hairy, stenotic or long steeply sloping ear canals

b) Trauma – Inappropriate cleaning using cotton buds etc. can cause physical damage to the delicate ear canal or ear drum
c) Concurrent disease – Other diseases may lead to the ear canals becoming more prone to the development of local disease
d) Lumps in the ear canal such as tumours, polyps or cysts. Happily these are relatively uncommon
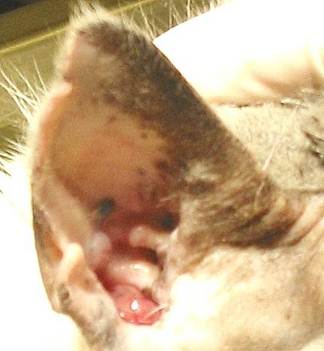
e) Moisture induced damage – quite common – resulting from persistent wetting e.g. swimming, leading to persistent conditions of high humidity in the ear

Factors that perpetuate an episode of otitis externa include those factors that exacerbate existing disease or prevent resolution of primary disease. These include:
a) Bacteria – A range of bacteria take advantage of existing damage and prolong it including Staphylococcus pseudintermedius, Pseudomonas aeruginosa and Proteus spp. These agents are generally considered as incapable of causing disease on their own.
b) Fungi – Malassezia pachydermatis – As for the bacteria above
c) Complicated ear disease – chronic narrowing, ulceration, the development of tumours or progression to deeper parts of the ear (middle ear)
d) Iatrogenic – the prolonged use of inappropriate ear medications or systemic antibiotics can lead to the development of resistant organisms which prolong disease as in a) above
Clinical Signs
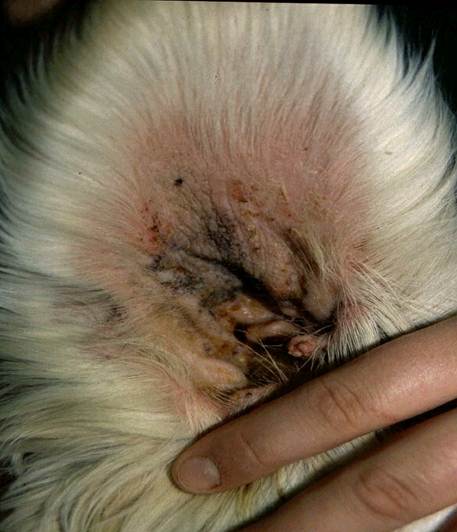
Clinical signs vary from mild to severe. The disease can begin as an animal holds its head to one side, shakes its head as if irritated and this can progress to the animal pawing at its ear(s). Disease is often bilateral. Animals can self-traumatise leading to scratched pinnae, or indeed even the development of an aural haematoma (reddish lump under the ear skin with thickening of the ear). Animals can experience quite a lot of pain and discomfort with this condition and early treatment for the relief of pain is warranted as well as dealing with the causal agents concerned. There may be visible exudate (discharge) present in and around the external ear canal which may or may not be accompanied by malodour (bad smell) from the ear.
Diagnosis

When the ear is inspected with an otoscope, the canal appears red and swollen in clinical cases. Touching or moving the outer ear increases the pain, and this manoeuvre on physical exam is important in establishing the clinical diagnosis. Your vet will be able to see the eardrum with an otoscope unless narrowing of the ear canal from inflammation and the presence of drainage and debris precludes this. A useful guide to the findings of otoscopic examination may be found by clicking here.
Both ears should be examined as the results are often quite different…indeed it is sensible if sampling is conducted that each ear is sampled separately.
Control
Your veterinary practitioner is best placed to advise you in this regard. However, the important steps are as follows:
a) Efficient cleaning is important initially as it allows the vet to observe the changes present and allows medication to work better along with facilitating removal of microbes/debris
b) Drying after cleaning is equally important – sedation or light anaesthesia may be required for these steps.
c) Otitis externa is invariably treated with topical medication. Antiparasitics may be included in the medication though a more common approach is for your vet to prescribe other medicines if parasites are suspected. Topical medications typically include:
1) Antimicrobial agents ideally selected based on culture and sensitivity of bacteria present. Commonly included antimicrobials include neomycin, gentamicin, polymixin B or fluoroquinolones
2) Antifungal compounds – Ask your vet about the different active ingredients as some are more effective than others e.g. azole compounds for Malassezia pachydermatis.
3) Anti-inflammatory compounds – Again, ask your vet about the different active ingredients as some are more effective than others at reducing pain.
Topical ear medicines containing ingredients against bacteria, fungi and inflammation are prescribed by your veterinary practitioner from whom advice must be sought.
Occasionally systemic treatment is justified especially in cases involving lack of response or otitis media. When the ear drum is ruptured, caution must be exercised with topical medications. Again, your local veterinary practitioner is best positioned to prescribe and advise on the use of suitable products.
