
Rabbit Haemorrhagic Disease
A page about viral haemorrhagic disease in rabbits describing cause, clinical signs, diagnosis and control.
Information
Rabbit haemorrhagic disease virus was first identified in China in 1984 and quickly spread to Europe from 1986-88. It is now endemic in most parts of world and is seen in all populations of rabbits (wild, pet and farmed).
Aetiology
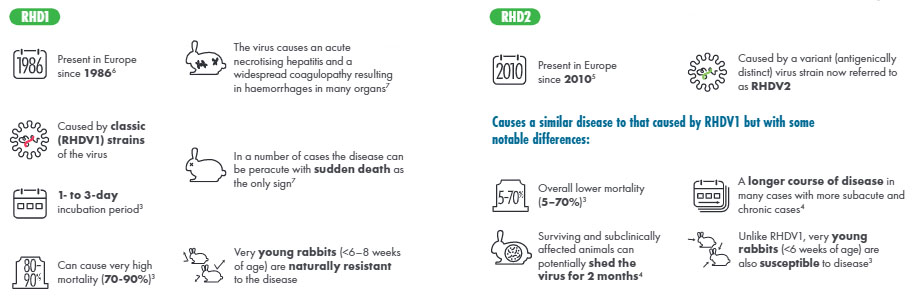
The causative agent of viral haemorrhagic disease is a calici virus called rabbit haemorrhagic disease virus. There are two recognised strains of this virus – RHD-1 and RHD-2.

Epidemiology
Rabbit haemorrhagic disease is highly contagious with transmission via oral, nasal or conjunctival routes. Infection most commonly happens through exposure to infected animal, carcass or fomites (food, bedding, water). Mechanical transmission may also be effected by insect vectors. The incubation period (time from initial exposure to onset of clinical signs) is 1-3 days
There are lots of ways your rabbits could pick up the virus:
Food (e.g. hay) or water contaminated by infected wild rabbits.
Birds or insects may bring the virus to your rabbits on their feet or in their droppings, which your rabbits may eat if they graze on the lawn.
The virus may be blown on the wind.
You (or your dog or cat) might accidentally bring the virus home on your feet from infected wild rabbit droppings, and vermin around rabbit hutches might bring it along too. You might pick it up from other peoples’ rabbits, for example at a show or even if another rabbit owner handles your rabbits.
The virus itself if extremely tough and can survive for many months in the environment, and can even resist temperatures of 60 degrees celsius. However, rabbits living indoors (house rabbits) are still at risk from VHD, so they definitely need to be vaccinated with boosters kept up to date.
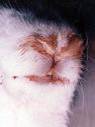
Clinical Signs
Disease severity and age groups affected depends on the strain involved. RHD-1 related disease is subclinical in young rabbits (<8-10 weeks old) but disease is likely to be severe and peracute in naive animals older than this. However, RHD-2 related disease is associated with lower mortality overall, yet very young rabbits are also susceptible to disease. The severity of disease is caused by widespread haemorrhages and hepatocellular degeneration with diffuse haemorrhages in many organs. A summary of the differences between clinical outcomes and other information concerning the two viral strains is outlined below. Three clinical syndromes exist:
Peracute: death (no clinical signs)
Acute:Fever
Nervous signs
Respiratory signs (dyspnoea, bloody nasal discharge)
Cyanosis of mucous membranes
Death in 12-36h
Chronic: Jaundice
Lethargy
Weight loss
Death in 1-2 weeks (liver dysfunction)
Diagnosis
Diagnosis may be suspected on clinical grounds but can only be confirmed by post mortem examination. Widespread haemorrhages on gross post mortem are highly suggestive.
Control
Control of viral haemorrhagic disease is based on three equally important aspects:
Biosecurity – Maintaining biosecurity involves avoiding introduction of animals into the group and/or implementing stict isolation / quarantine of introductions until proven free of disease, and restricting access of rabbits to external sources of infection – See hygiene below.
Hygiene – Good hygiene is very important in reducing the risk of disease, so keep hutches/cages very clean. Ensure that vermin and wild birds can’t get into outdoor hutches or runs. You might need to use weld-mesh with smaller holes! Make sure there is nothing attract to wild mice and rats to your rabbits: sweep up any spilt food and bedding. Don’t pick green foodstuffs from areas where wild rabbits live, and try to stop wild rabbits from getting into your garden. If this is not feasible, make sure it is impossible for wild visitors to have nose-to-nose contact with your pet rabbit.
Vaccination – To reduce risk of exposure is not sufficient alone to keep out infection and prevent it from continuing to spread. An additional control tool is to ensure animals are immune through vaccination. A combined vaccine against haemorrhagic disease and myxomatosis is available. This product may only be prescribed by your veterinary practitioner from whom advice must be sought.
Vaccination
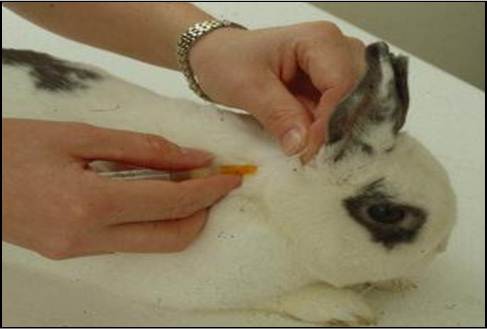
Vaccination is an important tool in ensuring the success of a control programme. A combined vaccine is available which is indicated for the control of myxomatosis and viral haemorrhagic disease.
Additional information on disease and vaccination is available by clicking here. For further information on the combined vaccine against myxomatosis and viral haemorrhagic disease (RHD-1 and RHD-2), please click here. It is always best to consult your local veterinary practitioner for best advice on disease control.
